
You're on your way!
You're being directed to a third-party site to get a quote.
Since 2011, we've helped more than 5 million visitors understand Medicare coverage.
By shopping with third-party insurance agencies, you may be contacted by a licensed insurance agent from an independent agency that is not connected with or endorsed by the federal Medicare program.
These agents/agencies may not offer every plan available in your area. Please contact Medicare.gov or 1-800-Medicare to get information on all options available.
After the Affordable Care Act (ACA) was passed in 2010, Medicare began to offer many preventive services without cost-sharing. Simply put, as long as your doctor accepts assignment (meaning they agree to charge no more than what Medicare allows) you get those services for free. What is surprising is how few people are taking advantage of this.
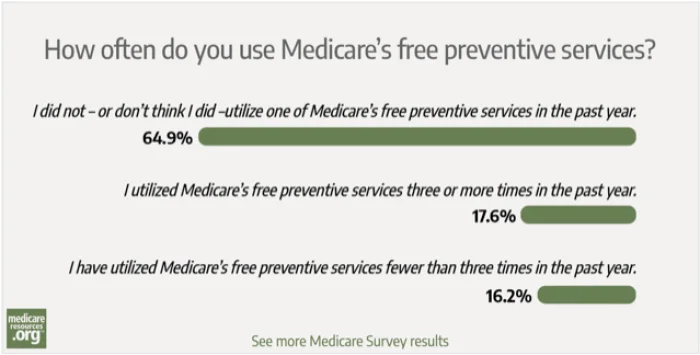
According to results from our latest Medicare Survey, nearly 65% of our readers hadn’t – or didn’t think they had – utilized one of Medicare’s free preventive services in the past year.
Here’s the actual survey question and results:
How often do you use Medicare’s free preventive services?
From a physician’s perspective, it’s worrisome to see such a significant percentage of Medicare enrollees missing out on a large number of free preventive services. These services range from cancer screenings (breast, cervical, colon, lung and prostate cancer) to vaccinations (COVID-19, hepatitis B, influenza, and pneumonia). Also free? Tests that check for abdominal aortic aneurysm, alcohol misuse, depression, diabetes, hepatitis C, HIV, osteoporosis, and sexually transmitted infections.
The Affordable Care Act also introduced the Annual Wellness Visit – free one-on-one time with your healthcare provider that allows you to go over your preventive care options.
(Other preventive services – including but not limited to diabetes self-training and glaucoma screening – will require enrollees to pay the 20% Part B coinsurance, although there are Medigap plans that will cover this cost.)
Some of these services are performed on a regular schedule, some are performed only once, and others are only offered for people considered to be at risk. Regardless of the service, they all offer significant health benefits.
By catching medical problems early on, they allow you to be treated sooner and will hopefully prevent future health complications. They have also been shown to improve your overall well-being and can help to reduce costs.
Medicare coverage is in alignment with screening guidelines set by the U.S. Preventive Services Task Force. The Task Force carefully reviews the available medical literature and only recommends services that have clinical benefits. You can be assured these tests are worth your time. The fact that many of them are free is an added bonus.
According to a 2020 study in the Journal of Policy Analysis and Management, the number of cancer diagnoses increases when people turn 65. This is not because people are suddenly getting cancer. It is because many of them are waiting to enroll in Medicare, a more affordable healthcare option than what they had before. Women, in particular, have been found to have a decreased risk for cancer mortality with this screening.
Interestingly, even though the use of preventive screening tests goes up once people go on Medicare those tests are still underutilized as a whole.
After the ACA passed, people began to attend Annual Wellness Visits (AWV) but the number was low. A 2019 review in Medical Care found that the number of AWVs increased from 8.1% in 2011 to 23.0% in 2016. That’s still less than one in four Medicare enrollees. Minorities were also less likely to attend these visits than non-Hispanic white beneficiaries.
The truth is that educating people about their preventive screening options matters. A 2019 study in the American Journal of Managed Care found that people who have Annual Wellness Visits are less likely to require hospital care – including emergency department visits – over the next 11 months. They also paid 5.7% less in healthcare costs during that time than their peers who did not have one of these preventive visits.
Although Medicare beneficiaries who have an AWV are counseled on their preventive screening options, that does not mean they actually go through with the recommended testing. Studies in BMC Health Services Research and Preventive Medicine have found that the number of cholesterol tests, colonoscopies, flu shots, mammograms, Pap smears, and prostate exams performed did not go up significantly after the ACA even though more people had an AWV.
It should not be surprising that the rates of office visits and preventive services decreased in the early months of the COVID-19 pandemic. Hospitals were busy caring for people infected with COVID-19. Elective procedures that are often performed at hospitals and ambulatory care centers, procedures like screening colonoscopies, were put on hold. More people turned to telehealth visits to decrease their risk for in-person COVID exposure but you can’t get a mammogram or Pap smear on the phone.
Office visits are back to near baseline levels now but some things haven’t changed. Preventive services are still underutilized. For example, the Centers for Disease Control and Prevention noted similar rates of flu shots pre-pandemic in 2019-2020 (56.2%) and during the pandemic in 2020-2021 (57.7%). Flu shot rates are actually lower at the same time this year (2021-2022 flu season) than they were last year.
The question is why are people choosing not to get preventive care, especially at a time when their health is at greater risk.
Part of the reason people defer screening may be that they do not understand what services are covered and when they are covered. The 2021 MITRE-Harris Poll Survey on health Insurance Literacy and Perception found that only a third of people with insurance, Medicare included, fully understand what preventive care services are covered by their plan.
There is also rising concern about surprise medical bills. The MITRE-Harris Survey found that 40% of people enrolled in Medicare received a bill that was larger than they expected and 38% received a bill for something they did not realize was not covered. This may make them hesitate to seek out certain services – especially if they do not realize that many of them are free.
When it comes to bills, it is also important to understand that the same test may be free in some circumstances but require cost-sharing in others. Preventive tests screen for conditions in people at risk. The goal is to find a disease early in its course before symptoms develop. Many of those tests are free. Diagnostic tests, on the other hand, are ordered by your doctor after you have symptoms. These tests are no longer considered preventive screening, and you will be charged for them. Keep in mind that any diagnostic services that are done during a preventive care visit may also require you to pay the Part B coinsurance.
Another issue may be that healthcare providers may not always talk about preventive care. Whether it is a sick visit or a visit to manage someone’s chronic medical problems, the amount of time allotted for each appointment limits how much time they have to address these other issues. A study in the Annals of Internal Medicine found that providers missed the opportunity to offer flu shots during an office visit that occurred during flu season more than 44% of the time.
Being aware of your options is key. Be sure to take a look at the Medicare & You Handbook mailed to you every year from the Centers for Medicare and Medicaid Services. Also, visit Medicare.gov and other reliable sources (including this site) to find out more about Medicare’s preventive care coverage.
Most importantly, reach out to your healthcare provider. I encourage you to book your free Annual Wellness Visit – your opportunity to go through your preventive screening options and to ask questions one on one. The visit is worth your time and can have a profound impact on your long-term health.
Tanya Feke, M.D. is a licensed, board-certified family physician living in New Hampshire. As a practicing primary care physician in Connecticut and an urgent care physician in New Hampshire, she saw first-hand how Medicare impacted her patients. In recent years, her career path has shifted to consultant work with a focus on utilization management and medical necessity compliance.
Dr. Feke is an expert in the field, having Medicare experience on the frontlines with patients, hospital systems, and insurers. To educate the public about ongoing issues with the program, she authored “Medicare Essentials: A Physician Insider Reveals the Fine Print.” Her analysis of Medicare issues is frequently referenced by the media, and she is a contributor to multiple online publications.