
You're on your way!
You're being directed to a third-party site to get a quote.
Since 2011, we've helped more than 5 million visitors understand Medicare coverage.
By shopping with third-party insurance agencies, you may be contacted by a licensed insurance agent from an independent agency that is not connected with or endorsed by the federal Medicare program.
These agents/agencies may not offer every plan available in your area. Please contact Medicare.gov or 1-800-Medicare to get information on all options available.
EDITOR’S NOTE: Our Medicare Surveys “take the pulse” of our audience – assessing our readers’ experiences with Medicare and their attitudes toward the program. The questions and the results are not intended to be scientific.
Our latest Medicare reader survey offers a reminder that the Medicare Part D system could use some improvements to make out-of-pocket costs more affordable for people who rely on multiple or expensive prescriptions. But it also highlights the fact that the majority of Medicare beneficiaries don’t comparison shop during open enrollment each year, and might be leaving money on the table as a result.
Most Medicare beneficiaries have prescription drug coverage, either via Medicare Part D (as a stand-alone plan or integrated with Medicare Advantage) or as part of an employer-sponsored plan for active employees or retirees. As of 2018, only about 12% of Medicare beneficiaries had no creditable drug coverage at all.
As of January 2021, there were 48.5 million beneficiaries with Part D coverage, accounting for about 77% of all Medicare beneficiaries. Part D coverage at that point was split nearly equally between stand-alone Part D plans, which covered 24.3 million people, and Medicare Advantage plans with integrated Part D benefits, which covered 24.2 million people (in terms of overall Medicare enrollment, nearly 43% of Medicare enrollees nationwide had Medicare Advantage plans, while the rest had Original Medicare).
The maximum allowable deductible for Part D coverage is $445 in 2021 (it will increase to $480 in 2022), although some plans have lower deductibles or no deductible at all, and it’s common for lower-tier drugs to be covered with copays even before the deductible is met. (For Medicare beneficiaries who rely on employer-sponsored drug coverage, benefit designs vary considerably from one employer to another.)
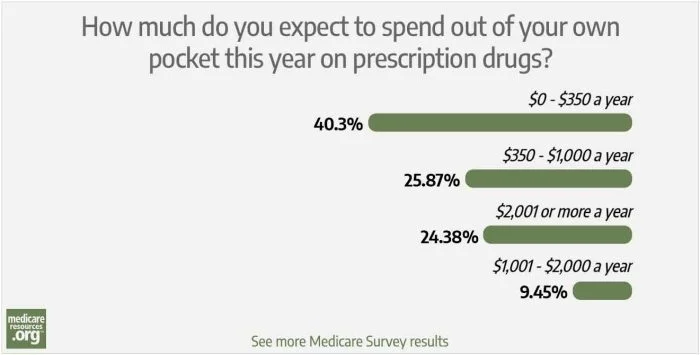
But enrollees’ coverage details vary greatly from one person to another, as do their medical needs. Our latest Medicare survey was designed to get at the actual amount that our readers are spending in out-of-pocket costs for their prescriptions, in addition to the premiums they pay for their coverage. Across more than 200 responses, this is what readers told us:
* note that these amounts don’t add to exactly 100%, due to rounding
So about two-thirds of our respondents expect to spend less than $1,000 this year at the pharmacy, while the other third expect to spend more than $1,000.
As of 2017, the average Part D enrollee (not counting those who qualify for Extra Help) had out-of-pocket costs that amounted to $486. Since then, overall prescription costs have increased – although some enrollees’ out-of-pocket costs for insulin are lower in 2021 – but the donut hole has also been eliminated (depending on the plan design, enrollees may still find that their costs increase once they reach the initial coverage limit, despite the fact that the Affordable Care Act has technically “closed” the donut hole). So we’re not surprised to see that the most commonly selected answer in our survey was “under $350” (especially since our respondents can include folks who qualify for Extra Help) and that the majority of our respondents expect to spend less than $1,000.
The 40% of our respondents who expect to spend less than $350 on prescriptions this year are likely a combination of folks who take few or no drugs (or only inexpensive generic medications) and those who qualify for Extra Help (ie, low-income subsidy for Part D coverage).
Many of these individuals either won’t meet their Part D deductible this year due to little in the way of prescription needs, or have low copays that remain at a very manageable level throughout the year.
What about the 26% of respondents who expect to spend between $350 and $1,000 at the pharmacy this year? If these folks have Part D coverage, they may or may not be hitting their deductibles. It depends on their drug needs and the coverage their plan provides. Many plans offer low copays for Tier 1 and Tier 2 drugs before the deductible is met, so a person might exceed $350 in drug spending via copays alone, without hitting the deductible.
For the folks who spend more than $1,000 but no more than $2,000 – amounting to roughly 10% of our respondents – the deductible is likely being met and they’re shifting to paying a copay or coinsurance each time they fill a prescription.
Only about a quarter of respondents expect to spend more than $2,000 on prescriptions this year. But although they account for the minority of our respondents, drug costs could be a significant financial burden for many of them. And unfortunately, this group also includes people whose prescription spending far exceeds $2,000, as Part D coverage does not have a cap on out-of-pocket costs. Beneficiaries who need high-cost specialty medications can find themselves in the catastrophic coverage level, where they continue to pay 5% of the cost of those medications for the remainder of the year.
A recent Kaiser Family Foundation analysis determined that 8% of Part D enrollees had drug costs that exceeded the catastrophic coverage level. Fortunately, the majority of those individuals were enrolled in Extra Help. But about a million enrollees who exceeded the catastrophic coverage level in 2017 did not receive assistance with their pharmaceutical bills, and there is no limit to how high their out-of-pocket costs can be.
Lawmakers are considering the possibility of including the Elijah E. Cummings Lower Drug Costs Now Act in the infrastructure bill that’s currently under consideration. This legislation would take a variety of actions to bring down drug costs for Medicare beneficiaries, including the introduction of a $2,000 cap on Medicare Part D out-of-pocket costs.
Although the addition of prescription drug coverage via Medicare Part D was a significant improvement to the Medicare system, consumer advocates have long noted the need for a cap on out-of-pocket spending. Without it, our system fails to adequately protect people whose income and/or assets exceed the limits for Extra Help, but whose prescription costs are still entirely unaffordable under the current Part D structure.
Even without new legislation, Medicare beneficiaries can save money on their prescriptions by simply comparison shopping each year during open enrollment. According to Kaiser Family Foundation research, well over half of all Medicare beneficiaries let their coverage auto-renew each year, without actively comparing the various options that are available to them.
If you’re not comparison shopping each year, you may be missing out on opportunities to switch to a plan that would provide better coverage for the medications you take. Your current plan might not be the best option anymore – maybe because your prescriptions have changed, maybe because your plan’s benefits have changed, or maybe because there are now other plans in your area that would be a better match for your prescription needs.
It’s also important to understand how your drug costs will vary depending on the pharmacy you use, so you’ll want to compare multiple pharmacies, including mail-order options, before you settle on a plan for the coming year. And if you enroll in a Medicare Advantage plan that includes Part D coverage, make sure you’re filling prescriptions at a preferred pharmacy in order to get the lowest out-of-pocket costs.
The good news is that you have an opportunity to switch plans each year, from October 15 to December 7. If you haven’t comparison shopped for the last few years, mark your calendar for the upcoming open enrollment period. You may find that your current plan is still the best option. But you also may find that a simple plan change could result in significant savings at the pharmacy next year.
Louise Norris is an individual health insurance broker who has been writing about health insurance and health reform since 2006. She has written dozens of opinions and educational pieces about the Affordable Care Act for healthinsurance.org. Her state health exchange updates are regularly cited by media who cover health reform and by other health insurance experts.